The placebo effect is the phenomenon of reported or observed medical improvement in the absence of an active treatment. The placebo effect in humans has been found in several studies of pain and depression, and a recent study even suggested that when Parkinson’s patients thought they were receiving an expensive treatment (saline), they showed more improvement in motor function than when they received what they thought was a cheaper treatment.

Now it might make sense that humans would be influenced by thinking they are receiving a treatment. If you’ve felt better in the past after taking a medication, perhaps you were then conditioned to equate a pill with feeling better. In the future, even a pill that has no active ingredient could help you feel better. This type of effect was seen in dogs who learned that being put into a chamber was followed by a morphine injection (these happened to be Pavlov’s dogs). Soon, just being placed in the chamber led to a similar physiological response before they even received the injection.
Can animals experience a placebo effect without any previous conditioning? That is a little harder to know without objective measures, because animals can’t report to us directly about how they are feeling. However, perhaps an animal’s human caregiver has something to say about how their pet feels?
There is a variation on the placebo effect known as the caregiver placebo effect, where family members or clinicians rate that someone receiving a placebo has improved; interestingly, often the family member or doctor rates the amount of improvement as higher than the patient themselves does. In some cases, the ratings of improvement by the caretaker also influence the self-report of the patient – somehow the behavior of others, who believe you are receiving treatment (and therefore perhaps are less anxious), makes you feel better too! This is called placebo-by-proxy. This effect has been studied in humans, but could it happen in our pets too?

A recent paper (Caregiver placebo effect in analgesic clinical trials for painful cats with naturally occurring degenerative joint disease) from a group in North Carolina, which included the fabulous pain specialist Duncan Lascelles, reviewed five studies of pain treatment of joint disease in cats, first looking at how caregivers reported improvement in the symptoms of their pet cats when the cats, unbeknownst to the human, received a placebo treatment. To look at whether there could be a caregiver placebo effect or a placebo-by-proxy effect, the paper compared the reported caregiver outcomes with objective measures of improvement. Let’s take a closer look.
Ninety-six cats participated in the five studies of joint pain. The treatments in the different studies were: a specialized diet, a nutraceutical, two studies of a nonsteroidal anti-inflammatory, and an anti-nerve growth factor antibody. Now would be a good time to note that the actual treatment in each study is of little importance because all of the data reported in the review is from placebo groups only! None of the data is from cats who were receiving an active treatment.
Cats were determined as having painful joint disease via orthopedic exams and x-rays. Each cat was then given a pain score. The objective outcome measure was the cat’s activity level as measured by an accelerometer. Each study also included a survey of the caregiver on the cat’s ease of doing different activities, such as walking, moving after resting, jumping, and finding a comfortable position.
The results compared owner report (O) of improvement in the survey against the objective measure of improvement (activity – A), meaning four possible combinations of outcomes: owner reports improvement (O+) and activity increases (A+); owner reports improvement, no activity increase (O+/A-); owner reports no improvement but activity increases (O-/A+); and owner reports no improvement and activity does not increase (O-/A-).
Let’s look at how results broke down and what they mean.
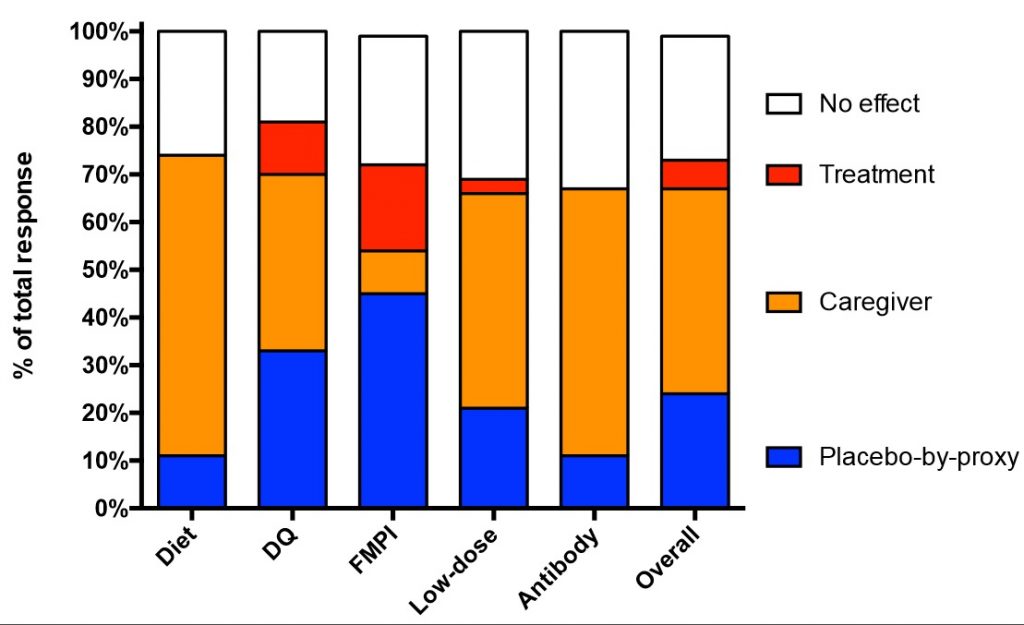
In 26% of all cases, neither the owner nor activity levels showed improvement (O-/A-). This would be considered a treatment failure. Only 6% of cats showed improvement independent of owner reports of improvement (O-/A+) – meaning that the cats increased their activity level but owner did not report improvement. Here is our objective measure of a true “treatment” effect, or the cats who may have improved anyway – so since there was no treatment, this suggests some waxing and waning of the disease, or cats who would have improved anyway.
Where things get interesting is when the humans reported improvement in their cats. Forty-three percent (!) of cats were subject to a caregiver placebo effect – where their human reported improvement but there was no increase in activity (O+/A-). These humans believed their cats were jumping and moving around with more ease. Their beliefs were not backed by the accelerometer data.
Finally, 24% of cats showed the placebo-by-proxy – where somehow the cats improved on objective measures apparently because the human thinks they are getting better! Perhaps these humans attended to their cats more, played with them more because they thought they might feel better, or just “wanted to believe.” Some of these cats may also be in the category of “regression to the mean” or extreme measures that would have gone back to normal levels – including cats who may have been at extremes of inactivity at the time the original activity measurement was taken.
There are several interesting things we must consider from this study. One is that perhaps the beliefs of the owner could have a positive effect on some cats. However, a large group of cats in this study experienced no objective improvement even though the owners felt they were better. This points out the importance of developing objective measures for outcomes for companion animals, because human beliefs may be to an extent, misreporting improvement. Those cats whose humans reported they improved, may have been suffering.
I’ve always found the placebo effect fascinating – the power of our beliefs to change our physiological systems demonstrates both the importance of our thoughts and the continuity rather than separation between brain and body – we must remember that the mind, the brain, and the body are all connected! However, when it comes to our animal companions, we have to make sure our judgments about their well-being aren’t clouded by our beliefs, so it appears that a future challenge will be making sure we have the tools we need to prevent that from happening.
To read more about the placebo effect in animals, this article by Dr. Frank McMillan and this blog post by the SkeptiVet are two good places to start!
Thank you to Dr. Tony Buffington for putting the graph together!



2 thoughts on “Is there such a thing as a “Purr-cebo Effect”?”
Comments are closed.