New research points to a strong placebo effect
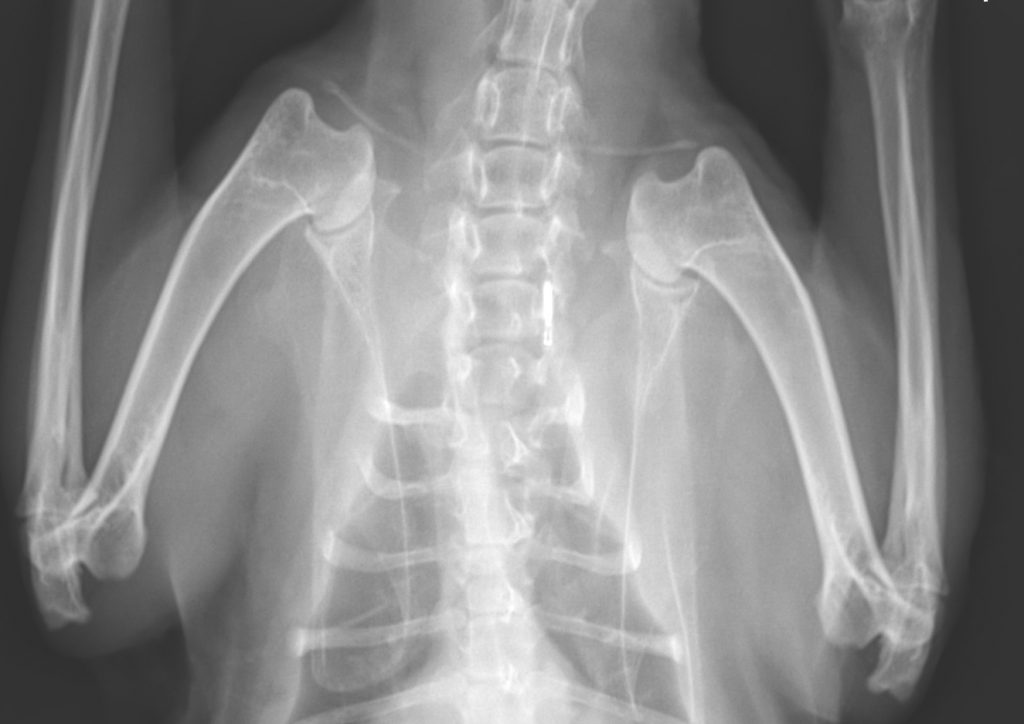
We take our knees and other joints for granted, but over time, joints are subject to wear-and-tear, as cartilage breaks down, and bones rub against each other. Ouch! Unfortunately, many cats also show signs of degenerative joint disease (DJD; also known as osteoarthritis), with multiple studies showing that over 90% of cats across all age ranges show some level of degeneration on radiographs (x-rays). DJD is a painful and chronic condition that can reduce mobility and impact a cat’s quality of life. True to its name, DJD is a progressive condition that becomes more severe over time.
In humans (and dogs), NSAIDs (non-steroidal anti-inflammatory drugs) are commonly prescribed to reduce pain and inflammation related to DJD. Unfortunately, cats are more likely to experience adverse side effects when given some NSAIDs, and so NSAIDs are more likely to be used short-term for pain with an acute onset, rather than a chronic pain condition, which requires ongoing treatment.
As a consequence, cats are more likely to be subscribed gabapentin or supplements, rather than medications such as Onsior or Metacam (both NSAIDs), which are approved for chronic pain in cats in some (but not all) areas of the world. Although gabapentin does seem to improve mobility for cats with DJD, it also can cause sedation. Joint supplements might be appealing as an alternative, and people often perceive them as “safe,” although they are often subjected to less research and evaluation compared to prescribed medications. The real question is, when it comes to pain, mobility, and a cat’s quality of life, do supplements actually DO anything?

Researchers at North Carolina State University recently compared the effects of the supplement Dasuquin for cats (containing glucosamine hydrochloride and chondroitin sulfate) with an identical placebo capsule to see if the Dasuquin would benefit the cats who received it. The study, “Evaluation of a nutritional supplement for the alleviation of pain associated with feline degenerative joint disease: a prospective, randomized, stratified, double-blind, placebo-controlled clinical trial,” was recently published in the Journal of Feline Medicine and Surgery.
The researchers hypothesized that cats on the supplement would have less pain and higher quality of life compared to cats receiving the placebo. In the name of full disclosure, it should be noted that Nutramax Labratories, the creator of Dasuquin, contributed to the study design and provided the supplements and placebo for the study.
The study was designed using the “gold standard” – meaning that both the cat owners and the veterinarians assessing the cats were blind to whether the cats were receiving a placebo or the supplement until the end of the study. Although cats were randomly assigned to conditions, the researchers also matched cats on severity of pain to ensure that the two groups were comparable. To participate in the study, cats had to be at least one year old, and show signs of DJD on examination and x-rays. The cats were otherwise healthy, although cats with mild kidney disease were allowed to participate.
At the start of the study, all cats received a physical examination, were assigned a pain score in response to palpation of all joints, and had blood work and urinalyses done. and their owners filled out a questionnaire about their cat’s activity and quality of life. All cats were fitted with an activity monitor on their collar.
For the first two weeks, all cats received a placebo. Then for six weeks, cats either received a placebo (30 cats) or supplement (29 cats). During that time, the cat’s owner was surveyed approximately every two weeks to assess their cat’s ability to perform different activities, and any changes they had observed in their cat’s quality of life. At the end of the study, cats were again examined by the veterinarian, including the pain assessment and lab work.
So how did the cats on Dasuquin do? Not how the researchers expected! Owners reported fewer signs of pain in cats who received the placebo, and there were no differences in reported activity or change in quality of life between the cats who received the supplement and those who received the placebo. All cats showed some improvement over time, whether based on owner report, or the veterinarian’s pain assessment. There were no differences in activity levels between the groups overall, although the least active cats tested did show more increases in activity if they received the supplement. The lab works remained stable over time in both groups of cats, who had similar values overall.
Interestingly, looking at the first two weeks of the study, when all cat owners unknowingly were giving their cat a placebo, 78% reported that their cat was already showing noticeable improvement. What does this mean? It’s likely that humans are very susceptible to a placebo effect. They think their cats feel better and are more active, although when assessed objectively, there’s very little evidence to support that. We see what we want to see. We want to see our cats feel better. I’ve written about the “purr-cebo” effect before (as reported in research by the same NC State research team) – it’s powerful stuff. But is it a problem?
Some might think that giving your cat supplements, herbal or homeopathic remedies, or something like CBD (which has not been tested for efficacy in cats for ANYTHING at this time) can’t hurt (after all, some of these things are actually INERT substances!). But if the choice is between giving your cat something that just downright doesn’t work versus giving them medication that could actually address the problem – whether it’s joint pain, symptoms of disease, or psychological symptoms such as anxiety – can you see why giving your cat a “harmless” pill can mean your cat does not receive the care they need?
The authors admit there’s plenty of room for future studies, including looking more closely at the less active cats who did seem to show some improvement on the supplement. Perhaps if the supplement was administered for a longer period, something would have happened. However, a large body of work in humans and dogs suggests inconsistent results, and overwhelmingly not a lot of strong evidence of the efficacy of glucosamine and chondroitin supplements.
Other studies have found more support for other supplements (including omega-3s) and new treatments are on the horizon – anti-nerve growth factor monoclonal antibodies appear very effective and were recently authorized in the EU. We can only hope that the United States follows and soon has more licensed options to treat painful cats. They deserve it, and their humans do too!
References
Cunningham, R., Gruen, M. E., Thomson, A., & Lascelles, B. D. X. (2021). Evaluation of a nutritional supplement for the alleviation of pain associated with feline degenerative joint disease: a prospective, randomized, stratified, double-blind, placebo-controlled clinical trial. Journal of feline medicine and surgery, 1098612X211053484.
Lascelles, B. D. X., Henry III, J. B., Brown, J., Robertson, I., Sumrell, A. T., Simpson, W., … & Pease, A. (2010). Cross‐sectional study of the prevalence of radiographic degenerative joint disease in domesticated cats. Veterinary surgery, 39(5), 535-544.

